So, let’s say you’re in the market for a home security system. The only one on the market has a few warnings on the label.
1. There is no guarantee that the system will work in case of a break in.
2. There is a chance that the electrical portion of the security system may start a serious fire in your home.
3. The system can not be un-installed.
Because the warnings are labeled on the package, neither the manufacturer nor distributor can not be held liable for any negative outcome.
Do you buy it or do you try to find an alternative way to defend your home?
By the way, your home is more likely to be broken into than you dying from a “vaccine preventable” illness, especially in a developed country with proper nutrition and access to medical care.
I completed extensive research on vaccines prior to my son’s birth. I researched the vaccines, their ingredients, their reported/unreported adverse actions, as well as the illnesses they were supposed to be protecting us against. I, personally, became resolved to the fact that the benefits do not outweigh the risks. Since then, many parents have asked my thoughts and personal opinion. Being that I don’t have personal experience with a vaccine injury, I can only give the information that I’ve accumulated.
The autism community is brimming with parents who believed in vaccinating their children at one time. These parents were considered “good parents” until their child had a horrible reaction to one of their routine vaccinations. Reactions can be anything from a fever or rash to full blown seizures. These parents had typically developing children until they reacted to a vaccine given at one of their well-baby visits….and their child was never the same again.
While my son has never been vaccinated, I am of the belief that vaccines can do harm to children who may have allergies, weakened immune systems or genetic susceptibility, such as an MTHFR mutation, or family history of autoimmune disorders. In my opinion, children should have certain tests done prior to any sort of vaccination, especially those with live viruses (ie MMR). As there are many scientific articles for the use of vaccinations, there are increasing reports and evidence to show that there is a link between vaccinations and autism, among other auto-immune related issues such as Type 1 Diabetes. The federal government has paid monies to at least 83 autism cases from the Vaccine Injury Compensation Program, despite stating that there is no link.
For more information, please see below:
Current recommended vaccination schedule
Vaccine Inserts from the CDC – This is a list of vaccines by brand name where you can see the inserts.
CDC: Who should not get vaccinated
Vaccine Ingredients (CDC Excipient list) updated Jan 2019
Vaccine Ingredients – This is important in that vaccines do contain ingredients, which are common allergens, such as yeast, eggs, soy or gelatin. Other known/questionable ingredients include formaldehyde, monosodium glutamate (MSG), and Thimerosal (a mercury containing organic compound). Nearly all vaccines contain a form of aluminum. Please note that single dose vials are safer as they do not contain preservatives. Multi-dose vials do contain preservatives.
Vaccine Ingredients2 – This article has calculated amounts of vaccine ingredients compared to FDA safety recommendations. For example, the FDA maximum requirements for aluminum received in an IV is 25mcg per day. The Hepatitis B shot has 250mcg in one shot, which can lead to central nervous system and bone toxicity. Excipient list from 2010.
CDC – Possible side effects of vaccines
Vaccine Safety Study: Placebo is as dangerous as the control because placebo is also a vaccine.
Vaccine AdverseEvent Reporting System
I strongly suggest reviewing information about each vaccine on the following website as it lists adverse effects that are not necessarily reported on the publicized websites. It also speaks of any laws that may be in place regarding vaccinations.
http://www.thinktwice.com/hpv.htm
US Dept of Health – Vaccine Injury Compensation Program Stats
DO NOT SIGN THE REFUSAL TO VACCINATE FORM
If you, or someone you know decides to vaccinate, please read below:
Why you should not give Tylenol to reduce a fever after vaccination
Tylenol reduces glutathione, which is the CHIEF antioxidant in the body, causing high risk for asthma.
Detox after a vaccination – For those who vaccinate, there are ways to help the body detox and get through the body’s reaction to the injected materials. This is only one link, as there are many suggestions. Here is another helpful link by Dr. Blaylock: http://www.rense.com/general87/vaccin.htm
Vaccine Shedding
Vaccination individuals transmitting whooping cough without having symptoms
Helpful Tips
Getting Antibody Titers Checked – Many vaccinations are given multiple times to ensure immunity, such as the MMR. One can measure their immunity level through a simple blood draw, prior to receiving another vaccination. If the immunity level is where it needs to be, the “booster” is not necessary.
Here is a Facebook page which lists professional, non-vax pushing and natural doctors by state.
Doctors who speak out against vaccines
Dr Green Mom – Find a Vaccine Friendly Doctor
Vaccine Efficacy
FDA state Pertussis Vaccine may not be effective
Eurosurveillance – shows that pertussis vaccine is not working in vaccinated children
Mayo Clinic – Paper states that measles vaccine is failing. Many are contracting the disease, even after receiving 2 doses of the immunization.
Reported Vaccine Efficacy
Religious Reasons to not get vaccinated
Biblical Reasons not to Vaccinate
Vaccination and Disease information:
True disease rates before and after vaccine introductions
Ready, Willing and unable to Serve – 75% of young adults cannot join the military due to mental/physical health disorders.
DTaP
Diptheria
Definition: An upper respiratory tract illness characterized by sore throat, low fever, and an adherent membrane on the tonsils, pharynx, and/or nasal cavity. A milder form of diphtheria can be restricted to the skin.
Symptoms: In its early stages, diphtheria can be mistaken for a bad sore throat. A low-grade fever and swollen neck glands are the other early symptoms.
Children infected have symptoms that include nausea, vomiting, chills, and a high fever, although some do not show symptoms until the infection has progressed further. In 10% of cases, patients experience neck swelling.
The toxin, or poison, caused by the bacteria can lead to a thick coating in the nose, throat, or airway. This coating is usually fuzzy gray or black and can cause breathing problems and difficulty in swallowing. The formation of this coating (or membrane) in the nose, throat, or airway makes a diphtheria infection different from other more common infections that cause sore throat.
As the infection progresses, the person may:
have difficulty breathing or swallowing
complain of double vision
have slurred speech
even show signs of going into shock (skin that’s pale and cold, rapid heartbeat, sweating, and an anxious appearance)
Where it comes from: People living in crowded or unclean conditions, those who aren’t well nourished.
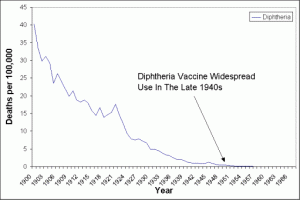
Stats: From 1900 to 1949, death rates from diphtheria declined from 40.3 per 100,000 to 0.4 per 100,000. The vaccine was introduced in 1949. In the United States, there were 52 reported cases of diphtheria between 1980 and 2000; between 2000 and 2007 there were only five cases. Fatality rates between 5% and 10%. In children under 5 years and adults over 40 years, the fatality rate may be as much as 20%. Mostly common in USSR. http://en.wikipedia.org/wiki/File:Diphterie.png
How you get it: Diphtheria is a contagious disease spread by direct physical contact or breathing the aerosolized secretions of infected individuals. It can also be spread to others who pick up tissues or drinking glasses that have been used by the infected person.
People who have been infected by the diphtheria bacteria can infect others for up to 4 weeks, even if they don’t have any symptoms. The incubation period (the time it takes for a person to become infected after being exposed) is 2-4 days, although it can range from 1 to 6 days.
Research suggests that although individuals immunized with an acellular pertussis vaccine may be protected from disease, they may still become infected with the bacteria without always getting sick and are able to spread infection to others, including young infants who are susceptible to pertussis disease. – FDA; 2013
How it’s treated: Children and adults with diphtheria are treated in a hospital. After a doctor confirms the diagnosis through a throat culture, the infected person receives a special anti-toxin, given through injections or through an IV, to neutralize the diphtheria toxin already circulating in the body, as well as antibiotics to kill the remaining diphtheria bacteria. After the antibiotics and anti-toxin have taken effect, someone with diphtheria will need bed rest for a while (4 to 6 weeks, or until full recovery).
Possible complications: In cases that progress beyond a throat infection, diphtheria toxin spreads through the bloodstream and can lead to potentially life-threatening complications that affect other organs of the body, such as the heart and kidneys. If the infection is advanced, people with diphtheria may need a ventilator to help them breathe. Patients may need intravenous fluids, oxygen, or heart medications. Bed rest is particularly important if the person’s heart has been affected by the disease. The toxin can cause damage to the heart that affects its ability to pump blood or the kidneys’ ability to clear wastes. It can also cause nerve damage, eventually leading to paralysis. Up to 40% to 50% of those who don’t get treated can die.
Tetanus
Definition: Also known as lockjaw, affects the body’s muscles and nerves. Generalized tetanus is the most common type of tetanus, representing about 80% of cases.
Where it comes from: Typically arises from a skin wound that becomes contaminated by a bacterium called Clostridium tetani, which is often found in soil. Tetanus occurs worldwide but is more common in hot, damp climates with soil rich in organic matter. More commin in Africa and Asian countries.
Symptoms: The first sign is lockjaw, and facial spasms followed by stiffness of the neck, difficulty in swallowing, and rigidity of pectoral and calf muscles. Other symptoms include elevated temperature, sweating, elevated blood pressure, and episodic rapid heart rate. Spasms may occur frequently and last for several minutes. Spasms continue for 3–4 weeks, and complete recovery may take months.
Neonatal tetanus is a form of generalized tetanus that occurs in newborn infants. It occurs in infants who have not acquired passive immunity from the mother. It usually occurs through infection of the unhealed umbilical stump, particularly when the stump is cut with a non-sterile instrument.
Stats: Fewer than 50 cases of tetanus are reported each year in the United States. Approximately 11% of reported tetanus cases have been fatal. The highest mortality rates are in persons over 60 years of age. Neonatal tetanus is common in many developing countries and is responsible for about 14% (215,000) of all neonatal deaths, but is very rare in developed countries.
How you get it: Any skin wound — especially a deep puncture or a wound that may be contaminated with feces, soil, or saliva. Tetanus is not contagious. The incubation period of tetanus ranges from 3 to 21 days, with an average onset of clinical presentation of symptoms in 8 days. In general, the further the injury site is from the central nervous system, the longer the incubation period. The shorter the incubation period, the higher the chance of death.
How it’s treated: A child who does develop tetanus will be treated in a hospital, usually in the intensive care unit (ICU). There, a child typically receives antibiotics to kill bacteria and Tetanus Immune Globulin (TIG) shot to neutralize the toxin that the bacteria have already released. This is important because many health care practitioners give the tetanus vaccine again, which will do nothing for a child that is already infected. The child will also receive medicines to control muscle spasms and may be given treatment to support vital body functions.
Possible complications: Laryngospasm (spasm of the vocal cords) is a complication that can lead to interference with breathing. Patients can also break their spine or long bones from convulsions. Other possible complications include hypertension, abnormal heart rhythm, and secondary infections, which are common because of prolonged hospital stays.
Pertussis (Whooping Cough)
Definition: An infection of the respiratory system caused by the bacterium Bordetella pertussis. It derived its name from the characteristic severe hacking cough followed by intake of breath that sounds like “whoop
Where it comes from: Common everywhere, highly contagious.
Symptoms: The first symptoms of whooping cough are similar to those of a common cold:
runny nose
sneezing
mild cough
low-grade fever
After about 1 to 2 weeks, the dry, irritating cough evolves into coughing spells. During a coughing spell, which can last for more than a minute, the child may turn red or purple. At the end of a spell, the child may make a characteristic whooping sound when breathing in or may vomit. Between spells, the child usually feels well. The last stage consists of another several weeks of recovery with gradual resolution of symptoms. In some children, the recovery period may last for months.
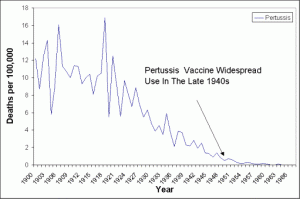
Stats: From 1900 to 1949, death rates from whooping cough declined from 12.2 per 100,000 to 0.5 per 100,000. The vaccine was introduced in 1949. Pertussis is the only disease that is associated with increasing deaths in the U.S.. The number of deaths increased from 4 in 1996 to 17 in 2001, almost all of which were infants under one year. See www.pertussis.com.
How you get it: Pertussis is highly contagious. The bacteria spread from person to person through tiny drops of fluid from an infected person’s nose or mouth. These may become airborne when the person sneezes, coughs, or laughs. Others then can become infected by inhaling the drops or getting the drops on their hands and then touching their mouths or noses. Infected people are most contagious during the earliest stages of the illness up to about 2 weeks after the cough begins. Antibiotics shorten the period of contagiousness to 5 days following the start of antibiotic treatment.
How it’s treated: The main treatment is care of sick children by observation, lifting them if they cough, preventing inhalation of vomit and feeding as necessary. Some children may need to be nursed in hospital. Treatment with an effective antibiotic shortens the infectious period but does not generally alter the outcome of the disease; however, when treatment is initiated during the catarrhal stage, symptoms may be less severe.
Close contacts who receive appropriate antibiotics during the 7–21 day incubation period may be protected from developing symptomatic disease. Close contacts are defined as anyone coming into contact with the respiratory secretions of an infected person in the 21 days before or after the infected person’s cough began.
Possible complications: Pneumonia, encephalitis, pulmonary hypertension, and secondary bacterial superinfection.
DTaP Vaccination complications: Three shots in one, which can be split up individually. The most common reactions are local reactions at the injection site, such as soreness, redness, and swelling, especially after the fourth or fifth dose. Other possible reactions may include fussiness, mild fever, loss of appetite, tiredness, and vomiting. The use of the more purified DTaP instead of the whole cell DTP has decreased these mild reactions substantially.
Side effects such as crying for three or more hours, high fever and encephalophathy have been known to occur. People who had a serious allergic reaction to a previous dose of DTaP or Tdap vaccine, or who developed encephalopathy (brain injury), not due to another identifiable cause, should not receive another dose.
Certain rare adverse events following pertussis vaccination usually serve as a precaution against receiving further doses. Such events include a temperature of 105°F or higher, collapse or shock-like state, persistent crying for more than three hours, or convulsions within three days.
The DTap vax is not 100% efficient, which is why there are several boosters required through the age of 5. In addition, the vaccine loses efficacy over time, thus teens and adults need boosters to really be effective. The adult version, TDap, only protects about 7/10 people. So you can get the vaccination, but still get whooping cough and pass it on to others. This is actual info from the CDC. http://www.cdc.gov/pertussis/about/faqs.html
Rota
Rotavirus
Definition: It is the leading, single cause of severe diarrhea among infants and young children. There are seven species of this virus, referred to as A, B, C, D, E, F and G. Rotavirus A, the most common, causes more than 90% of infections in humans.
Where it comes from: Rotavirus is transmitted by the fecal-oral route, via contact with contaminated hands, surfaces and objects and possibly by the respiratory route. The feces of an infected person can contain more than 10 trillion infectious particles per gram; only 10–100 of these are required to transmit infection to another person.
Symptoms: Vomiting, watery diarrhea, and low-grade fever. Once a child is infected by the virus, there is an incubation period of about two days before symptoms appear. Symptoms often start with vomiting followed by four to eight days of profuse diarrhea. Dehydration is more common in rotavirus infection than in most of those caused by bacterial pathogens, and is the most common cause of death related to rotavirus infection.
Stats: By the age of five, nearly every child in the world has been infected with rotavirus at least once. However, with each infection, immunity develops, subsequent infections are less severe, and adults are rarely affected.
How you get it: Rotavirus is transmitted by the fecal-oral route, via contact with contaminated hands, surfaces and objects and possibly by the respiratory route.
How it’s treated: Treatment of acute rotavirus infection is nonspecific and involves management of symptoms and, most importantly, maintenance of hydration. Depending on the severity of diarrhea, treatment consists of oral rehydration with plain water, water plus salts, or water plus salts and sugar.
Possible complications: If untreated, children can die from the resulting severe dehydration. Some infections are serious enough to warrant hospitalisation where fluids are given by intravenous drip or nasogastric tube, and the child’s electrolytes and blood sugar are monitored. Rotavirus infections rarely cause other complications and for a well managed child the prognosis is excellent. There are rare reports of complications involving the central nervous system (CNS) where rotavirus was detected in the fluid of the CNS in cases of encephalitis and meningitis.
Rota Vaccination Complications: Children are slightly (1 to 3 percent) more likely to have mild, temporary diarrhea or vomiting within 7 days after getting a dose of rotavirus vaccine than children who have not gotten the vaccine. Moderate or severe reactions have not been associated with this vaccine.
MMR
Mumps
Definition: Mumps is a disease affecting salivary glands, often causing them to swell and become painful. These glands, which produce saliva for the mouth, are found toward the back of each cheek, in the area between the ear and jaw.
Where it comes from: Caused by a virus that usually spreads through saliva and can infect many parts of the body, especially the parotid salivary glands.
Symptoms: Cases of mumps may start with a fever of up to 103° Fahrenheit (39.4° Celsius), as well as a headache and loss of appetite. The well-known hallmark of mumps is swelling and pain in the parotid glands, making the child look like a hamster with food in its cheeks. The glands usually become increasingly swollen and painful over a period of 1 to 3 days. The pain gets worse when the child swallows, talks, chews, or drinks acidic juices (like orange juice).
Stats: Since 2001, the case average was only 265 per year, excluding an outbreak of >6000 cases in 2006 attributed largely to university contagion in young adults
How you get it: The mumps virus is contagious and spreads in tiny drops of fluid from the mouth and nose of someone who is infected. It can be passed to others through sneezing, coughing, or even laughing. The virus can also spread to other people through direct contact, such as picking up tissues or using drinking glasses that have been used by the infected person. Highly contagious for up to 3 weeks before and 4 weeks after symptoms. Being close to a person with the mumps in this period makes you likely to attract the virus even with an MMR vaccine.
How it’s treated: There is no specific treatment for mumps. Because mumps is caused by a virus, it cannot be treated with antibiotics. You can also soothe your child’s swollen parotid glands with either warm or cold packs. Serve a soft, bland diet that does not require a lot of chewing and encourage your child to drink plenty of fluids. Avoid serving tart or acidic fruit juices (like orange juice, grapefruit juice, or lemonade) that make parotid pain worse. Water, decaffeinated soft drinks, and tea are better tolerated. Children usually recover from mumps in about 10 to 12 days. It takes about 1 week for the swelling to disappear in each parotid gland, but both glands don’t usually swell at the same time.
Possible complications: Death is very unusual. Mumps can lead to inflammation and swelling of the brain and other organs, although this is not common. Encephalitis (inflammation of the brain) and meningitis (inflammation of the lining of the brain and spinal cord) are both rare complications of mumps.
Known complications of mumps include:
Infection of other organ systems
Sterility in men (this is quite rare, and mostly occurs in older men)
Mild forms of meningitis (rare, 40% of cases occur without parotid swelling)
Encephalitis (very rare, rarely fatal)
Profound (91 dB or more) but rare sensorineural hearing loss, uni- or bilateral
Pancreatitis manifesting as abdominal pain and vomiting
Oophoritis (inflammation of ovaries) but fertility is rarely affected.
Measles – 14 things to consider about measles
Definition: A highly contagious respiratory infection that’s caused by a virus.
Where it comes from: The measles is a highly contagious airborne pathogen.
Symptoms: The first symptoms of the infection are usually a hacking cough, runny nose, high fever, and red eyes. A characteristic marker of measles are Koplik’s spots, small red spots with blue-white centers that appear inside the mouth. The measles rash typically has a red or reddish brown blotchy appearance, and first usually shows up on the forehead, then spreads downward over the face, neck, and body, then down to the arms and feet.
Stats: From 1900 to 1963, death rates from measles had declined from 13.3 per 100,000 to 0.2 per 100,000. The vaccines was introduced in 1963. The fatality rate from measles for otherwise healthy people in developed countries is low: approximately 1 death per thousand cases. In underdeveloped nations with high rates of malnutrition and poor healthcare, fatality rates of 10 percent are common.
How you get it: Spreads primarily via the respiratory system. The virus is transmitted in respiratory secretions, and can be passed from person to person via aerosol droplets containing virus particles, such as those produced by a coughing patient. A person with measles is contagious from 1 to 2 days before symptoms start until about 4 days after the rash appears.
How it’s treated: Since measles is caused by a virus, there is no specific medical treatment and the virus has to run its course. But a child who is sick should be sure to receive plenty of fluids and rest, and be kept from spreading the infection to others.
Possible complications: Complications with measles range from relatively mild and less serious diarrhea, to pneumonia and encephalitis, corneal ulceration leading to corneal scarring. Complications are usually more severe among adults who catch the virus.
Rubella
Definition: Commonly known as German measles or 3-day measles — is an infection that primarily affects the skin and lymph nodes. This disease is often mild and attacks often pass unnoticed.
Where it comes from: There is no carrier state: the reservoir exists entirely in active human cases. Rubella is a disease that occurs worldwide. The virus tends to peak during the spring in countries with temperate climates.
Symptoms: Rubella infection may begin with 1 or 2 days of mild fever (99–100°) and swollen, tender lymph nodes, usually in the back of the neck or behind the ears. A rash then appears that begins on the face and spreads downward. As it spreads down the body, it usually clears on the face. This rash is often the first sign of illness that a parent notices. The rubella rash can look like many other viral rashes. It appears as either pink or light red spots, which may merge to form evenly colored patches. The rash can itch and lasts up to 3 days. As the rash clears, the affected skin occasionally sheds in very fine flakes. The rubella rash typically lasts 3 days. Lymph nodes may remain swollen for a week or more, and joint pain can last for more than 2 weeks. Children who have rubella usually recover within 1 week, but adults may take longer.
Stats: In 2004, there were only nine rubella cases reported in the United States.
How you get it: rubella is transmitted via airborne droplet emission from the upper respiratory tract of active cases. The virus may also be present in the urine, feces and on the skin. The disease has an incubation period of 2 to 3 weeks. The rubella virus passes from person to person through tiny drops of fluid from the nose and throat. People who have rubella are most contagious from 1 week before to 1 week after the rash appears. Someone who is infected but has no symptoms can still spread the virus.
How it’s treated: There is no specific treatment; management is a matter of responding to symptoms to diminish discomfort. Treatment of newly born babies is focused on management of the complications.
Possible complications: Serious complications are very rare.
MMR Vaccination Complications: 3 shots in one, which can be split up individually.
Mild Problems: Fever (up to 1 person out of 6), Mild rash (about 1 person out of 20), Swelling of glands in the cheeks or neck.
If these problems occur, it is usually within 7-12 days after the shot. They occur less often after the second dose.
Moderate Problems: Seizure (jerking or staring) caused by fever (about 1 out of 3,000 doses), temporary pain and stiffness in the joints, mostly in teenage or adult women (up to 1 out of 4), temporary low platelet count, which can cause a bleeding disorder (about 1 out of 30,000 doses).
Severe Problems: Serious allergic reaction includes rash; hives; itching; difficulty breathing; tightness in the chest; swelling of the mouth, face, lips, or tongue; pain, redness, or swelling at the injection site; swelling of the glands in the jaw; swelling of the testicles.
Long Term Severe Problems: Deafness, Long-term seizures, coma, or lowered consciousness, Encephalitis – (swelling of the brain) Permanent brain damage.
Many parents report that their perfectly healthy children became autistic after receiving the MMR vaccine. Please see http://www.thinktwice.com for more info.
HepB
Hepatitis B
Definition: A virus that infects the liver, causing inflammation.
Symptoms: Half of all people infected with the hepatitis B virus have no symptoms.
Symptoms develop within 30-180 days of exposure to the virus. The symptoms are often compared to flu. Most people think they have flu and never think about having HBV infection.
Appetite loss
Fatigue
Nausea and vomiting
Itching all over the body
Pain over the liver (on the right side of the abdomen, under the lower rib cage)
Jaundice – A condition in which the skin and the whites of the eyes turn yellow in color
Urine becomes dark in color (like cola or tea).
Stools are pale in color (grayish or clay colored).
How you get it: Transmission of hepatitis B virus results from exposure to infectious blood or body fluids containing blood. Possible forms of transmission include (but are not limited to) unprotected sexual contact, blood transfusions, re-use of contaminated needles & syringes, and vertical transmission from mother to child during childbirth.
How it’s treated: Acute hepatitis B infection does not usually require treatment because most adults clear the infection spontaneously. Chronically infected individuals are candidates for therapy. Although none of the available drugs can clear the infection, they can stop the virus from replicating, and minimize liver damage such as cirrhosis and liver cancer. Currently, there are seven medications licensed for treatment of hepatitis B infection in the United States.
Possible complications: Having a chronic HBV infection eventually may lead to serious liver diseases such as cirrhosis and liver cancer. Having had HBV infection as an infant or child gives you a greater chance of developing these illnesses as an adult. In addition, hepatitis B puts you at risk of acute liver failure — a condition in which all the vital functions of the liver shut down. When that occurs, a liver transplant is necessary to sustain life.
HepB Vaccination Complications:
Mild problems: Soreness where the shot was given, lasting a day or two, mild to moderate fever (up to 1 out of 14 children and adolescents and 1 out of 100 adults).
Severe problems: Serious allergic reaction
The hepatitis B vaccine has been linked to immunological and neurological disorders. Please see http://www.thinktwice.com for more info.
Statistics have found that U.S. male neonates vaccinated with the hepatitis B vaccine have a threefold higher risk of receiving an autism diagnosis compared to boys not vaccinated as neonates.
http://www.ncbi.nlm.nih.gov/pubmed/21058170
HepA
Hepatitis A
Definition: A virus that infects the liver, causing inflammation. The risk of infection is greatest in developing countries with poor sanitation or poor personal hygiene standards.
Symptoms: Many people with HAV infection have no symptoms at all. Sometimes symptoms are so mild that they go unnoticed. Older people are more likely to have symptoms than children. People who do not have symptoms can still spread the virus.
Symptoms of hepatitis A usually develop between 2 and 6 weeks after infection. The symptoms are usually not too severe and go away on their own, over time. The most common symptoms are as follows:
Nausea
Vomiting
Diarrhea, especially in children
Low-grade fever
Loss of appetite
Rash
Tiredness, fatigue
Jaundice – A yellow discoloration of the skin and the whites of the eyes
Urine is dark brownish in color, like cola or strong tea.
Pain in area of liver – On the right side of the abdomen, just under the rib cage
Symptoms usually last less than two months, although they may last as long as nine months. About 15% of people infected with hepatitis A have symptoms that come and go for 6-9 months.
How you get it: The hepatitis A virus is found in feces is transmitted through fecal-oral transmission. If food or drinking water becomes contaminated with stool from an infected person (usually because of inadequate hand washing or poor sanitary conditions), the virus can quickly spread to anyone who drinks or swallows the contaminated food or water. The virus can also be spread by eating raw or undercooked shellfish collected from water that has been contaminated by sewage. The hepatitis A virus can be transmitted through blood transfusions, although this is extremely rare.
How it’s treated: There are no specific medicines to cure infection with hepatitis A. Most people require no treatment except to relieve symptoms. If you have been exposed to someone who is infected with HAV, there is a treatment that may prevent you from becoming infected. It is called immune globulin and is more likely to be effective when given within 2 weeks of exposure. In most cases of hepatitis A, the liver heals completely in a month or two with no lasting damage. Furthermore, the virus doesn’t remain in your body once you’ve recovered.
Possible complications: Older adults and people with other medical problems, such as congestive heart failure, diabetes and anemia, may take longer to recover and are likely to have a more serious course of the disease. In rare cases, fulminant hepatitis — a life-threatening condition that causes liver failure may develop. Especially at risk are people with chronic liver disease or a liver transplant. In addition, some studies suggest that the inflammation triggered by hepatitis A may contribute to atherosclerosis — the gradual buildup of hardened deposits in your arteries.
Hep A Vaccination Complications:
Mild problems: soreness where the shot was given, headache (about 1 out of 6 adults and 1 out of 25 children), loss of appetite (about 1 out of 12 children), fatigue (about 1 out of 14 adults)
If these problems occur, they usually last 1 or 2 days.
Severe problems: serious allergic reaction, within a few minutes to a few hours of the shot. The severe side effects are the same for any allergic reaction to medicines including high fever, breathing abnormality, hoarseness, wheezing, dizziness and elevated heart beat.
IPV
Inactivated Polio Virus
Definition: Contagious disease caused by an intestinal virus that may attack nerve cells of the brain and spinal cord.
Where it comes from: It is seasonal in temperate climates, with peak transmission occurring in summer and autumn. These seasonal differences are far less pronounced in tropical areas.
Symptoms: Although around 90% of polio infections cause no symptoms at all, affected individuals can exhibit a range of symptoms if the virus enters the blood stream. Early symptoms of paralytic polio include high fever, headache, stiffness in the back and neck, asymmetrical weakness of various muscles, sensitivity to touch, difficulty swallowing, muscle pain, loss of superficial and deep reflexes, paresthesia (pins and needles), irritability, constipation, or difficulty urinating. Paralysis generally develops one to ten days after early symptoms begin, progresses for two to three days, and is usually complete by the time the fever breaks.
The term poliomyelitis is used to identify the disease caused by any of the three serotypes of poliovirus. Two basic patterns of polio infection are described: a minor illness which does not involve the central nervous system (CNS), sometimes called abortive poliomyelitis, and a major illness involving the CNS, which may be paralytic or non-paralytic. In most people with a normal immune system, a poliovirus infection is asymptomatic. Rarely the infection produces minor symptoms; these may include upper respiratory tract infection (sore throat and fever), gastrointestinal disturbances (nausea, vomiting, abdominal pain, constipation or, rarely, diarrhea), and influenza-like illnesses.
Stats: The Americas were declared polio-free in 1994. In 2000 polio was officially eradicated in 36 Western Pacific countries, including China and Australia. Europe was declared polio-free in 2002.[75] As of 2006, polio remains endemic in only four countries: Nigeria, India, Pakistan, and Afghanistan.
How you get it: The disease is transmitted primarily via the fecal-oral route, by ingesting contaminated food or water. It is occasionally transmitted via the oral-oral route, a mode especially visible in areas with good sanitation and hygiene. Polio is most infectious between 7–10 days before and 7–10 days after the appearance of symptoms, but transmission is possible as long as the virus remains in the saliva or feces. The time between first exposure and first symptoms, known as the incubation period, is usually 6 to 20 days, with a maximum range of 3 to 35 days.[13] Virus particles are excreted in the feces for several weeks following initial infection.
Several studies have shown that injections (for antibiotics or other vaccines) increase susceptibility to polio. In 1995, the New England Journal of Medicine published a study showing that children who received a single injection within one month after receiving a polio vaccine were 8 times more likely to contract polio than children who received no injections. The risk jumped 27-fold when children received up to nine injections within one month after receiving the polio vaccine. And with ten or more injections, the likelihood of developing polio was 182 times greater than expected. Why injections increase the risk of polio is unclear.
How it’s treated: There is no cure for polio. The focus of modern treatment has been on providing relief of symptoms, speeding recovery and preventing complications. Supportive measures include antibiotics to prevent infections in weakened muscles, analgesics for pain, moderate exercise and a nutritious diet. Treatment of polio often requires long-term rehabilitation, including physical therapy, braces, corrective shoes and, in some cases, orthopedic surgery. Individuals who are exposed to the virus, either through infection or by immunization with polio vaccine, develop immunity.
Possible complications: Encephalitis, an infection of the brain tissue itself, can occur in rare cases and is usually restricted to infants. It is characterized by confusion, changes in mental status, headaches, fever, and less commonly seizures and spastic paralysis. The virus enters the central nervous system in about 3% of infections. Most patients with CNS involvement develop non-paralytic aseptic meningitis, with symptoms of headache, neck, back, abdominal and extremity pain, fever, vomiting, lethargy and irritability. Approximately 1 in 200 to 1 in 1000 cases progress to paralytic disease, in which the muscles become weak, floppy and poorly-controlled, and finally completely paralyzed; this condition is known as acute flaccid paralysis. Depending on the site of paralysis, paralytic poliomyelitis is classified as spinal, bulbar, or bulbospinal.
The likelihood of developing paralytic polio increases with age, as does the extent of paralysis. In children, non-paralytic meningitis is the most likely consequence of CNS involvement, and paralysis occurs in only 1 in 1000 cases. In adults, paralysis occurs in 1 in 75 cases. In children under five years of age, paralysis of one leg is most common; Paralysis rates also vary depending on the serotype of the infecting poliovirus; the highest rates of paralysis (1 in 200) are associated with poliovirus type 1, the lowest rates (1 in 2,000) are associated with type 2.
IPV Vaccination Complications: In countries using IPV, no increased risk for serious adverse events has been observed. Possible side effects include minor local reactions at the site of injection (e.g., pain, redness).
Anyone who has ever had a life-threatening allergic reaction to neomycin, streptomycin, or polymyxin B should not get the IPV shot because it contains trace amounts of these antibiotics.
There is evidence that the polio vaccine actually increased the rates of polio. In 1977, Dr Jonas Salk, the man who developed the first polio vaccine, testified along with other scientists that mass inoculation against polio was the cause of most polio cases throughout the USA since 1961. (Science 4/4/77 “Abstracts” ). Polio was already on a natural decline when the vaccination was introduced, by way of better hygiene, diet and sanitation. In addition, the Polio vaccine used at that time had traces of the SV 40 virus which is directly linked to the creation of cancer within the body. Many adults now, who were vaccinated as children, believe they are experiencing the effects of that cancer causing virus right now.
PCV
Pneumococcal
Definition: Pneumococcal disease is caused by Streptococcus pneumoniae, a bacterium. There are more than 90 subtypes. Most subtypes can cause disease, but only a few produce the majority of invasive pneumococcal infections. The 10 most common subtypes cause 62% of invasive disease worldwide. There are three major conditions caused by invasive pneumococcal disease: pneumonia, bacteremia, and meningitis. They are all caused by infection with the same bacteria, but have different symptoms.
Symptoms:
Pneumococcal pneumonia (lung disease) is the most common disease caused by pneumococcal bacteria. It is estimated that 175,000 hospitalizations due to pneumococcal pneumonia occur each year in the United States. The incubation period is short (1-3 days). Symptoms include abrupt onset of fever, shaking chills or rigors, chest pain, cough, shortness of breath, rapid breathing and heart rate, and weakness. The fatality rate is 5%-7% and may be much higher in the elderly.
Pneumococcal bacteremia (blood infection) occurs in about 25%-30% of patients with pneumococcal pneumonia. More than 50,000 cases of pneumococcal bacteremia occur each year in the United States. Bacteremia is the most common clinical presentation among children younger than age two years, accounting for 70% of invasive disease in this group.
Pneumococci cause 13%-19% of all cases of bacterial meningitis (infection of the covering of the brain or spinal cord) in the United States. There are 3,000-6,000 cases of pneumococcal meningitis each year. Symptoms may include headache, tiredness, vomiting, irritability, fever, seizures, and coma. Children younger than age one year have the highest rate of pneumococcal meningitis, approximately 10 cases per 100,000 population. The case fatality rate is high (30% overall, up to 80% in the elderly).
Pneumococci are also a common cause of acute otitis media (middle ear infection). Approximately 28%-55% of such ear infections are caused by S. pneumoniae. In the U.S., there are 4.9 million cases of otitis media each year in children younger than age five years. Middle ear infections are the most frequent reason for pediatric office visits in the United States, resulting in more than 20 million visits annually.
Stats: Case-fatality rates are highest for meningitis and bacteremia, and the highest mortality occurs among the elderly and patients who have underlying medical conditions. Before a vaccine was available in the United States, pneumococcal disease caused serious disease in children younger than age five years. Each year it was responsible for causing 700 cases of meningitis, 17,000 blood infections, five million ear infections, and 200 deaths. Children younger than age two years are at the highest risk for serious pneumococcal disease. Healthcare providers are not required by law to report pneumococcal disease to health authorities, so exact numbers are not known. Estimates have been made from a variety of population studies, however, and it is believed that 45,000 cases of invasive pneumococcal disease (meningitis and blood infections) occur each year in the United States. (Pneumonia and middle ear infections are most common but are not considered “invasive” diseases.) The incidence of the disease varies greatly by age group. The highest rate of invasive pneumococcal disease occurs in young children, especially those younger than age two years. Children with certain chronic diseases (e.g., sickle cell disease or HIV infection) are at very high risk of invasive disease.
How you get it: The disease is spread from person to person by droplets in the air. The pneumococci bacteria are common inhabitants of the human respiratory tract. They may be isolated from the nasopharnyx of 5%-70% of normal, healthy adults. The exact period of communicability is not known. It appears that transmission can occur as long as the organism remains in respiratory secretions.
How it’s treated: Penicillin is the drug of choice for treatment of pneumococcal disease; however, resistance to penicillin and other antibiotics has been on the rise. Studies indicate that in some areas of the United States up to 40% of invasive pneumococci are resistant to common antibiotics. Treating patients infected with resistant organisms requires expensive alternative antimicrobial agents and may result in prolonged hospital stays. The increased difficulty of treating this serious bacterial infection makes prevention through vaccination even more important.
Possible complications:
You can get pneumococcal disease more than once.
There are more than 90 known subtypes of pneumococcus bacteria, with 23 subtypes included in the current pneumococcal polysaccharide (adult) vaccine and 7 subtypes included in the current conjugate (child) vaccine. Having been infected with one type does not always make the patient immune to other types. Even if an individual has had one or more episodes of invasive pneumococcal disease, he or she needs to be vaccinated.
PCV Vaccination Complications: In studies (nearly 60,000 doses), pneumococcal conjugate vaccine (for children) was associated with only mild reactions:
Up to about 1 infant out of 4 had redness, tenderness, or swelling where the shot was given.
Up to about 1 out of 3 had a fever of over 100.4 degrees Fahrenheit, and up to about 1 in 50 had a higher fever (over 102.2 degrees Fahrenheit).
Some children also became fussy or drowsy, or had a loss of appetite.
It is noted that there appears to be a large number of seizures reported by male children, though both male and female reports exist in the 2007 database of VAERS. We have found that hospitalization/ER visits were common within the first 3 days, 14 days, and 30 days after the injection.
Hib
Haemophilus Influenzae type b4
Definition: H. influenzae is responsible for a wide range of clinical diseases. Most strains of H. influenzae usually live in their host without causing disease, but cause problems only when other factors (viral infection or reduced immune function) create an opportunity. There are six generally recognized types of H. influenzae: a, b, c, d, e, and f.
Where it comes from: Can be found in the upper respiratory system of humans.
Symptoms: Symptoms vary based on the disease. In infants and young children, H. influenzae type b (Hib) causes bacteremia, pneumonia, and acute bacterial meningitis. Occasionally, it causes cellulitis, osteomyelitis, epiglottitis, and joint infections. Unencapsulated H. influenzae (non-B type) causes ear (otitis media) and eye (conjunctivitis) infections and sinusitis in children, and is associated with pneumonia.
How you get it: The H. influenzae bacteria live in the upper respiratory tract and are usually transmitted by close contact with an infected individual. Droplets in the air from a sneeze can be inhaled and may also cause infection.
How it’s treated: Treatment for H. influenzae greatly depends on which area of the body is infected. Specific treatment for H. influenzae will be determined by your child’s physician based on: your child’s age, overall health, and medical history, extent of the disease, your child’s tolerance for specific medications, procedures, or therapies, expectations for the course of the disease, your opinion or preference.
Regardless of the location, antibiotics may be used to treat infections caused by H. influenzae. The length of treatment varies depending on the location and severity of the infection. Other therapy will be supportive (aimed at treating the symptoms present).
Possible complications: Depends on which area of the body is infected
Hib Vaccination Complications:
Mild Problems
Redness, warmth, or swelling where the shot was given (up to 1 out of 4 children)
Fever over 101 degrees Fahrenheit (up to 1 out of 20 children)
If these problems happen, they usually start within a day of vaccination. They may last 2-3 days.
Serious problems associated with receiving the immunization are rare and are mainly allergic reactions to vaccine components.
Varicella
Chickenpox
Definition: Highly contagious illness generally begins with a vesicular skin rash.
Where it comes from: seen throughout the year but more commonly in winter and early spring.
Symptoms: The chicken pox lesions (blisters) start as a two to four millimeter red papule which develops an irregular outline . A thin-walled, clear vesicle (dew drop) develops on top of the area of redness. After about 8 to 12 hours the fluid in the vesicle becomes cloudy and the vesicle breaks leaving a crust. The crust usually falls off after seven days sometimes leaving a crater-like scar. Although one lesion goes through this complete cycle in about seven days, another hallmark of chickenpox is that new lesions crop up every day for several days. Therefore it may be a week before new lesions stop appearing and existing lesions crust over. Children should not be sent back to school until all lesions have crusted over.
How you get it: Chickenpox is a highly contagious disease that spreads from person to person by direct contact or by air from an infected person’s coughing or sneezing. Touching the fluid from a chickenpox blister can also spread the disease. A person with chickenpox is contagious from one to five days before the rash appears. The contagious period continues until all blisters have formed scabs, which may take 5 to 10 days. It takes from 10 to 21 days after contact with an infected person for someone to develop chickenpox.
How it’s treated: There is no evidence to support the effectiveness of topical application of calamine lotion, a topical barrier preparation containing zinc oxide in spite of its wide usage and excellent safety profile. It is important to maintain good hygiene and daily cleaning of skin with warm water to avoid secondary bacterial infection. An oatmeal bath also might help ease discomfort. Following primary infection there is usually lifelong protective immunity from further episodes of chickenpox.
Possible complications: Chickenpox is rarely fatal, although it is generally more severe in adults than in children.
Varicella Vaccination Complications:
Mild Problems: Soreness or swelling where the shot was given (about 1 out of 5 children), Fever (1 person out of 10, or less), Mild rash, up to a month after vaccination (1 person out of 20, or less).
It is possible for these people to infect other members of their household, but this is rare.
Note: MMRV vaccine has been associated with higher rates of fever (up to about 1 person in 5) and measles-like rash (about 1 person in 20) compared with MMR and varicella vaccines given separately.
Moderate Problems: Seizure (jerking or staring) caused by fever (less than 1 person out of 1,000).
Severe Problems: Pneumonia
Other serious problems, including severe neurological problems (brain reactions) and low blood count, have been reported after chickenpox vaccination.
The vaccine can cause herpes zoster (shingles). The risk of zoster following vaccination appears to be less than that following infection with the varicella virus. The majority of cases of shingles following vaccine have been mild and have not been associated with serious complications. Persons with weakened immune systems and those with life-threatening allergies to gelatin or the antibiotic neomycin should not receive this vaccine.
MCV4
Meningococcal
Definition: Medical condition that is caused by inflammation of the protective membranes covering the brain and spinal cord. The inflammation is usually caused by infection with viruses, bacteria, or other microorganisms but may also arise due to certain drugs, or other diseases. Meningitis is potentially life threatening due to the inflammation’s proximity to the brain and spinal cord; it is therefore a medical emergency.
Where it comes from: Meningitis is usually caused by infection by microorganisms. Seen mostly in Africa, Asia and South America.
Symptoms: The most common symptoms of meningitis are headache and neck stiffness associated with fever, confusion or altered consciousness, and an inability to tolerate bright light or loud noises. Sometimes, especially in small children, only nonspecific symptoms may be present, such as irritability and drowsiness. If a rash is present, it may indicate a particular cause of meningitis; for instance, meningitis caused by meningococcus bacteria may be accompanied by a characteristic rash.
Stats: Populationwide rates of bacterial meningitis declined significantly from 1.9 cases per 100,000 people in 1998 to 1.5 per 100,000 in 2003.
How you get it: Most cases are due to infection with viruses, followed by bacteria, fungi, and parasites. Viruses that can cause meningitis include various enterovirus subtypes, herpes simplex virus 2 (and less commonly HSV-1), varicella zoster virus (known for causing chickenpox and shingles), mumps virus and HIV.
How it’s treated: Meningitis must be treated promptly with antibiotics and sometimes antiviral drugs. In some situations, corticosteroid drugs can also be used to prevent complications from overactive inflammation.
Possible complications: Meningitis can lead to serious long-term consequences such as deafness, epilepsy, hydrocephalus and cognitive deficit, especially if not treated quickly.
MCV4 Vaccination Complications:
Mild problems: Up to about half of people who get meningococcal vaccines have mild side effects, such as redness or pain where the shot was given. These usually last for 1 or 2 days. They are more common after MCV4 than after MPSV4.
A small percentage of people who receive the vaccine develop a fever.
Severe problems: Serious allergic reactions, within a few minutes to a few hours of the shot. A serious nervous system disorder called Guillain-Barré Syndrome (or GBS) has been reported among some people who received MCV4.
HPV
Human Papillomavirus
Definition: Genital human papillomavirus (HPV) is the most common sexually transmitted infection (STI). The virus infects the skin and mucous membranes. There are more than 40 HPV types that can infect the genital areas of men and women, including the skin of the penis, vulva (area outside the vagina), and anus, and the linings of the vagina, cervix, and rectum.
Symptoms: Most people with HPV do not develop symptoms or health problems. But sometimes, certain types of HPV can cause genital warts in men and women. Other HPV types can cause cervical cancer and other less common cancers, such as cancers of the vulva, vagina, anus, and penis. The types of HPV that can cause genital warts are not the same as the types that can cause cancer.
Stats: Approximately 20 million Americans are currently infected with HPV, and another 6.2 million people become newly infected each year. At least 50% of sexually active men and women acquire genital HPV infection at some point in their lives.
How you get it: Genital HPV is passed on through genital contact, most often during vaginal and anal sex. A person can have HPV even if years have passed since he or she had sex. Most infected persons do not realize they are infected or that they are passing the virus to a sex partner.
How it’s treated: There is no treatment for the virus itself, but a healthy immune system can usually fight off HPV naturally. There are treatments for the diseases that HPV can cause:
Visible genital warts can be removed by patient-applied medications, or by treatments performed by a health care provider. Some individuals choose to forego treatment to see if the warts will disappear on their own. No one treatment is better than another.
Cervical cancer is most treatable when it is diagnosed and treated early. There are new forms of surgery, radiation therapy, and chemotherapy available for patients [see http://www.cancer.org ]. But women who get routine Pap testing and follow up as needed can identify problems before cancer develops. Prevention is always better than treatment.
Other HPV-related cancers are also more treatable when diagnosed and treated early. There are new forms of surgery, radiation therapy, and chemotherapy available for patients. [see http://www.cancer.org ]
Possible complications: High-risk viruses cause cervical cancer and also are associated with vulvar cancer, anal cancer, and cancer of the penis (a rare cancer). Although most HPV infections do not progress to cancer.
Genital warts may cause a number of problems during pregnancy. Sometimes they enlarge during pregnancy, making urination difficult. If the warts are on the vaginal wall, they can make the vagina less elastic and cause obstruction during delivery.
Rarely, infants born to women with genital warts develop laryngeal papillomatosis (warts in the throat). Although uncommon, it is a potentially life-threatening condition for the child, requiring frequent laser surgery to prevent obstruction of the airways. Research on the use of interferon therapy in combination with laser surgery indicates that this drug may show promise in slowing the course of the disease.
HPV Vaccination Complications:
Several mild problems may occur with HPV vaccine:
Pain at the injection site (about 8 people in 10)
Redness or swelling at the injection site (about 1 person in 4)
Mild fever (100 degrees Fahrenheit) (about 1 person in 10)
Itching at the injection site (about 1 person in 30)
Moderate fever (102 degrees Fahrenheit) (about 1 person in 65)
These symptoms do not last long and go away on their own.
There have been 42 reported deaths in the United States from receiving this vaccination and nearly 6 million dollars has been paid out to families due to injury or death from this vaccine. Japan has suspended its recommendations of the vaccine for young girls due to numerous adverse side effects.
The above information was determined from the following sources:
Wikipedia, the free encyclopedia
Books
What Your Doctor May Not Tell You About Childhood Vaccines
Helpful Websites